NHS calls for more black blood donors to help treat sickle cell disease
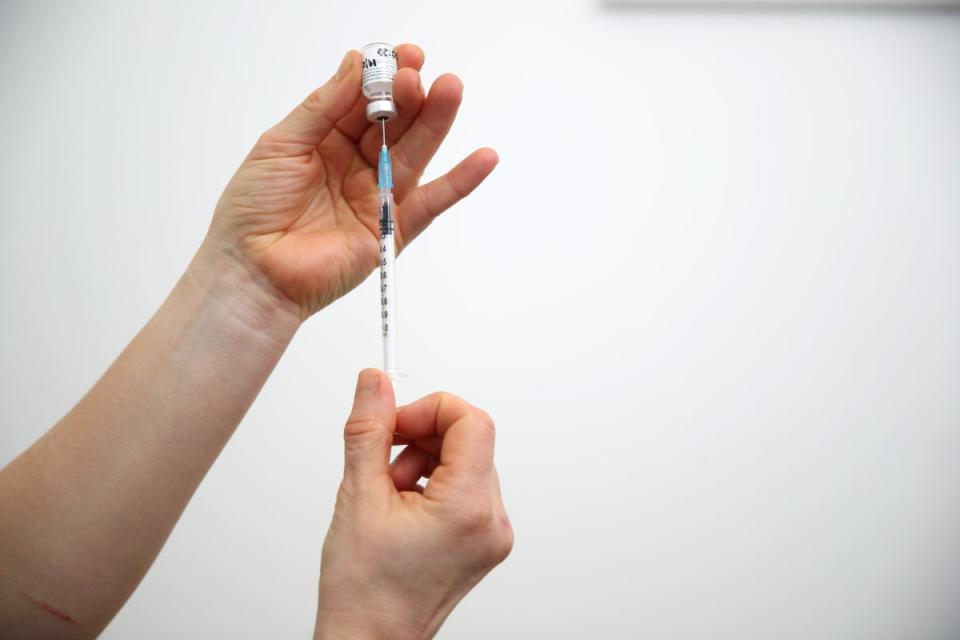
NHS Blood and Transplant (NHSBT) is urging the public to give blood, as demand for blood donations continues to rise.
Blood donations are needed now more than ever to treat people with sickle cell disease and demand has risen by around 67 per cent over the past five years.
Sickle cell is a blood disease that disproportionately affects people of African or Caribbean heritage and has become the fastest growing genetic condition in the UK.
It works by causing red blood cells to form into sickle or crescent shapes and become stuck in blood vessels, causing agonising crisis episodes, and serious or even fatal long-term complications including organ damage and strokes. Many patients need frequent blood transfusions just to stay alive.
Around 250 donations are needed daily to help people with sickle cell, up from 150 donations five years ago. This demand stems from patients living longer and the increase in complete blood transfusions which improve results for patients.
Currently, the NHS is only able to provide transfusions that match patients’ blood types just over half the time, which leaves other patients being treated with the universal blood type, O negative, which, though clinically safe, can eventually lead to complications.
Around 55 per cent of black people have a Ro blood type, compared to two per cent of the wider population.
ââYou can become a blood donor via the Give Blood NHS app or on the NHS Blood and Transplant website.
Lanre Ogundimu, from South London, has sickle cell and almost died in 2018 from an adverse reaction to a blood donation.
Although the major blood groups were matched, she reacted to a minor blood group and the lack of ethnically matched blood increases the risk of these reactions.
Ogundimu, a radio producer, told Sky: “I can’t receive blood as a standard treatment any more. Well-matched blood from within the black community can be the difference between life or death.”
Cherrelle Lawrence, a senior biomedical scientist at NHSBT’s blood-matching lab in London, said: “Matched blood is vital for sickle-cell patients to reduce the risk of serious complications. People from the same ethnic background are more likely to have matching blood.
“There is a rise in black people donating blood, but we urgently need more to become regular donors. Giving blood is easy, quick, and safe - and you will save and improve lives.”

 Yahoo Sport
Yahoo Sport 




































